Published in Ophthalmic Surgery, Lasers & Imaging. Surgical Management of Inner Lamellar Macular Holes. 2007 Jan-Feb 38(1):61-3
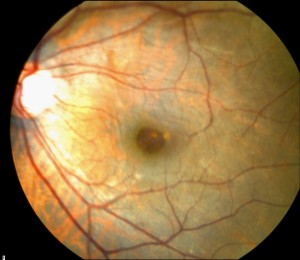
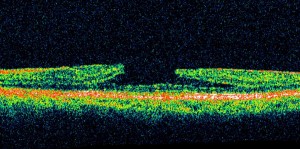
Lamellar Macular Hole traditionally has been considered a non-surgical problem, although full-thickness macular holes are commonly treated. This patient presented with symptoms of blurred vision and metamorphopsia in their eft eye. The fundus photography (see Figure 1) and OCT (see Figure 2) are typical of a lamellar macular hole with a round defect in the retina, which is not full thickness, as well as a partial thickness defect in the retina with overhanging edges on the OCT.
Figure 1 (pre-operative) Fundus Photograph
Figure 2 (pre-operative) OCT Scan
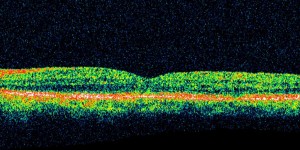
Pars plana vitrectomy with membrane peeling and placement of air with face down positioning for only 2 days resulted in marked improvement in symptoms and improvement of visual acuity to 20/25. Surprisingly, OCT showed an almost normal recovery of the foveal contour and resolution of the inner lamellar macular hole (see Figure 3).
Figure 3 (post-operative) OCT Scan
This case is one of the first reported cases to demonstrate a potentially successful surgical approach to this condition. This case was reported to the Macula Society and American Society of Retina Specialists in 2006.